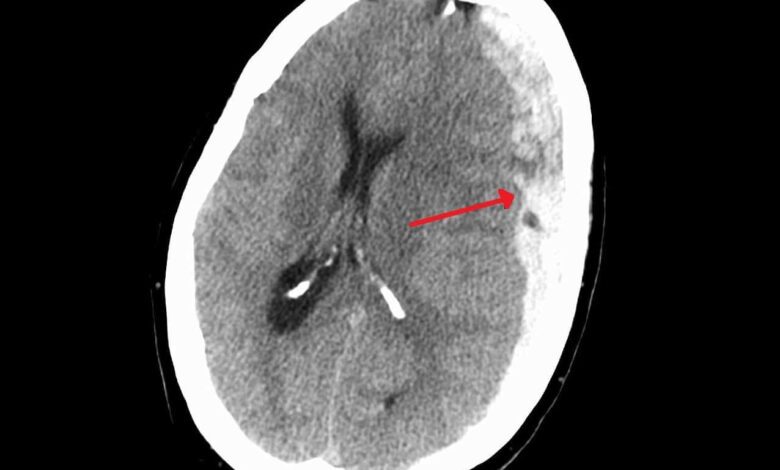
A subdural hematoma is one of the most dangerous complications following head injuries, especially in the elderly. Bleeding beneath the brain’s membranes often leads to severe consequences, and diagnosis is complicated by the fact that its symptoms can mimic other age-related conditions. Doctors note that even minor blows in patients taking blood-thinning medications can result in serious complications.
The mortality rate for such injuries remains high: according to statistics, up to 14% of patients do not survive, and a significant proportion of survivors are left with disabilities. The problem is compounded by the fact that chronic hematomas can appear weeks after the injury, masquerading as dementia or stroke.
In a situation where treatment outcomes are difficult to predict, specialists from Perm (Wagner Perm State Medical University and PNIPU) set out to identify objective criteria for assessing patients’ prognoses. They analyzed medical records of individuals admitted to the hospital within six hours of injury and divided them into groups based on hematoma location: frontotemporal, parietotemporal, and frontoparietooccipital regions.
The results showed that the location of the hemorrhage directly affects the chances of recovery. The most favorable outcomes were observed in patients with frontal-temporal hematomas—this group was the most likely to regain independent living. In contrast, when the frontal-parietal-occipital area was affected, the prognosis worsened significantly: these patients arrived in a more severe condition, and the hematoma volume was greater.
A comparison of young and elderly patients with the same hemorrhage volume revealed a significant difference in outcomes. According to the modified Rankin Scale, where each point reflects the loss of independence, elderly patients were discharged with higher scores, indicating a need for constant daily assistance. The difference was particularly striking in cases with parietal-temporal hematoma.
An additional risk factor for elderly people was taking anticoagulants prior to injury: all such patients required support after discharge. Modern treatment guidelines help determine the approach—surgery or conservative therapy—but do not answer the question of the chance for returning to previous quality of life.
To fill this gap, scientists have developed a digital tool that enables rapid assessment of recovery prospects. A doctor enters key parameters into the program: age, hematoma size and location, the time from injury to admission, and information about any blood-thinning medications the patient is taking. The algorithm analyzes the data and provides a prognosis: favorable, moderate, or unfavorable.
The main advantage of the system is that it can be used in the first hours after an injury, when every minute counts. The program does not require specialized equipment and can be implemented in any emergency room. It helps doctors make decisions and explain to families what to expect from treatment, relying on objective data.
Currently, the digital assistant is already being used in clinical practice and continues to improve. This development opens new opportunities for a personalized approach to treating severe head injuries and could become a standard in emergency medicine.












