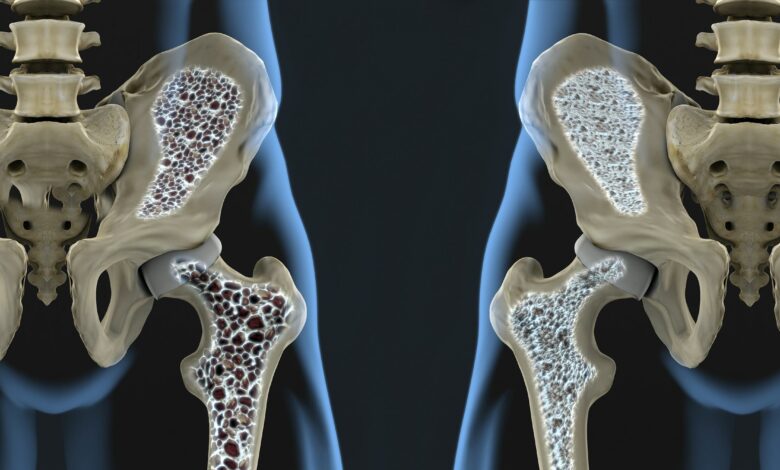
Loss of bone mass and decreased skeletal strength are serious issues affecting millions of people, especially the elderly. Osteoporosis leads to frequent fractures and requires long-term treatment, while current medications often cause side effects or provide only temporary relief.
An international team of specialists from Leipzig University has introduced an innovative approach that could change this landscape. Through their experiments, researchers identified the key role of the GPR133 receptor, which is responsible for activating the cells that form bone tissue. This G protein-coupled receptor triggers a signaling cascade that promotes the maturation of osteoblasts—the cells responsible for building bone.
To activate GPR133, researchers used the AP503 molecule, which significantly boosted bone formation in laboratory mice. In animal experiments involving subjects with osteoporosis, AP503 led to a marked increase in bone density and volume. At the same time, in mice lacking the GPR133 gene, the drug had no effect, confirming its targeted action.
Particular attention was given to modeling conditions similar to menopause in women, when decreased estrogen levels cause bones to become fragile. Administration of AP503 helped restore the balance between bone destruction and formation, and also increased the number of active osteoblasts.
The mechanism of this new method is based on boosting the intracellular cAMP signal, which activates enzymes and helps stabilize beta-catenin—a protein essential for triggering genes responsible for bone growth. As a result, precursor cells turn into mature osteoblasts more quickly, making bone structure stronger and healthier.
Despite these impressive results, researchers still face several challenges. So far, tests have only been conducted on animals, whose bone structure and renewal rates differ from those of humans. Before beginning clinical trials, it is necessary to thoroughly study the drug’s safety, determine the optimal dosage, and rule out unwanted side effects.
Another crucial question is whether prolonged activation of the receptor can support bone growth without risking calcium deposits in other organs. In addition, GPR133 is part of a large receptor family, so achieving high selectivity is essential to avoid unintended effects on other body systems.
Given the genetic differences among individuals, the researchers plan to investigate how patients with different GPR133 gene variants respond to the new drug. This will help identify those who would benefit most from the treatment.
If further trials confirm the method’s effectiveness and safety, doctors will have a fundamentally new tool to combat osteoporosis. This approach can not only strengthen bones, but also help patients maintain their activity and independence for years to come.










